“We’ve all got a terminal disease, it’s called life.” – Benedict Groeschel
Few people know what it’s like to live with a terminal illness. For those who do, the experience can be both harrowing and enlightening. This article will explore the process of dying and the different ways that people cope with a terminal illness. It will also discuss the importance of support systems during this difficult time. Finally, the post will provide advice for those who are supporting someone with a terminal illness. Let’s get started.
- What is a terminal illness?
- Can a terminal illness be cured?
- What are the most common terminal illness?
- How do you know if you or someone you love has a terminal illness?
- How painful is terminal illness?
- What happens after the diagnosis of a terminal illness?
- Are the symptoms the same during the final days?
- What are the phases of dying?
- What happens when you are actively dying?
- What are the 7 stages of grief/dying?
- How do families cope with a loved one who is terminally ill?
- What are the options for those who are terminally ill?
- What is hospice care and how does it work?
- Tips for someone facing death?
- How do I deal with grief and loss?
What is a terminal illness?
A terminal illness is a medical condition that cannot be cured and is expected to result in death. Some scholars refer to terminal illness as having a life expectancy of 6 months or less (Hui et al., 2013).
The transition from managing illness to preparing for death is challenging.
tyrrell et al., 2022
Can a terminal illness be cured?
No, a terminal illness cannot be cured. Treatment for a terminal illness may focus on symptom management and providing comfort, but it is not expected to cure the underlying condition.
People with a terminal illness often have a limited life expectancy and may require hospice care to manage their symptoms and provide support for themselves and their families.
What are the most common terminal illness?
The most common terminal illnesses include advanced cancer, heart failure, organ failure, and neurological disorders.
How do you know if you or someone you love has a terminal illness?
There is no single answer to this question, as each individual and situation is unique. However, there are some common signs and symptoms that may indicate a terminal illness, which include:-
- Experiencing severe and/or worsening pain that is not responding to treatment
- Losing the ability to perform basic activities of daily living (e.g., eating, bathing, dressing)
- Developing new and unexplained physical symptoms
- Experiencing significant psychological distress (e.g., anxiety, depression, hopelessness)
If you are concerned that you or someone you love may have a terminal illness, it is important to seek professional medical help. A doctor can provide a diagnosis and discuss treatment options and prognosis.
It is also important to keep in mind that not all terminal illnesses are immediately life-threatening, and some people may live for many years with a terminal diagnosis. If you have any questions or concerns, please don’t hesitate to speak with your doctor.
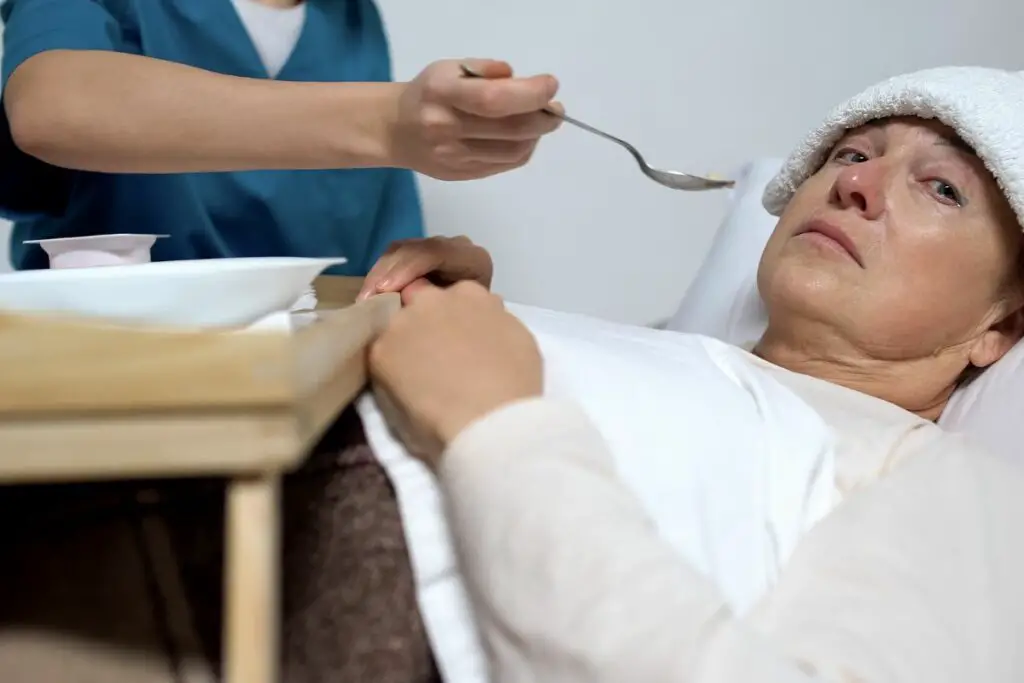
How painful is terminal illness?
Terminal illness can be very painful, depending on the individual and their condition. However, there are many treatments available to help manage symptoms and reduce pain.
It is important to discuss any concerns with your doctor so that they can provide the best care possible.
What happens after the diagnosis of a terminal illness?
Usually, after the diagnosis of a terminal illness, the patient and health care professional try to slow the progression of the disease and extend their life.
Later, the patient often considers hospice care, when they stop seeking treatment and focus on making the most of their remaining time.
Terminal illnesses are often unpredictable, so it is important to be prepared to better cope with the challenges of a terminal diagnosis.
Are the symptoms the same during the final days?
No, the symptoms experienced during the final days of a terminal illness can vary significantly depending on the individual and their condition. Some people may experience severe pain, while others may only have minor visible discomfort.
It is also important to note that some individuals may remain alert and relatively active until nearing death, while others may become more sedentary as their illness progresses.
Therefore, it is important to closely monitor the individual’s condition and stay in contact with their doctor to ensure they receive the best possible care.
What are the phases of dying?
The stages of dying are typically divided into two phases: pre-active, and active.
Pre-active phase of dying
During the pre-active phase, individuals may experience changes in their physical health or emotional state as they adjust to their diagnosis. This stage usually lasts for weeks or months. According to an article by Crossroads Hospice & Palliative care (2022), this stage typically lasts 3 weeks.
Active phase of dying
The active phase is then marked by a progressive decline in health, typically with an increase in symptoms and physical weakness. Death usually occurs during the active phase. Some scholars claim that the active stage lasts about 3 days (Crossroads Hospice & Palliative care, 2022).
What happens when you are actively dying?
Actively dying is the last stage of a terminal illness and typically occurs shortly before death. Symptoms during this stage can include:
- difficulty breathing
- decreased alertness
- significantly decreased blood pressure
- incontinence (urinary and bowel)
- loss of appetite
- accumulation of fluids in lungs (gurgling sounds)
- physical weakness
- hallucinations or delirium
- rigidity
Actively dying is the final hours/days when physiological functions decline and death is imminent.
kintzel et al., 2012
Notably, all patients will not have all of these signs. Some persons may even state that they are dying (Crossroads Hospice & Palliative Care, 2022). Treatment at this point focuses on providing comfort to the individual and their loved ones.
What are the 7 stages of grief/dying?
According to Kubler-Ross, there are seven stages of dying. Notably, Kubler-Ross initially identified 5 stages, commonly known as the DABDA model. These included Denial, Anger, Bargaining, Depression, and Acceptance (Tyrrell et al., 2022).
Since then, the stages were revised and two additional stages have been identified: shock and testing. Hope is important for each stage and helps the person get through these challenging times (Perring, no date).
| Stage of Grief/Dying | Characteristics |
|---|---|
| Shock | Initial response. Confusion and disbelief. Emotional Paralysis. |
| Denial/Isolation | A feeling of shock and disbelief experienced by most persons. Shock is usually temporary. Isolation results from avoidance from other persons – even family members. May slip in and out of this stage based on life/disease evolution and coping skills. |
| Anger | Feeling a sense of injustice or frustration. May be directed towards God, health care professional, family members etc. May result in jealousy of others. |
| Bargaining | Attempting to make deals with an outside force in order to delay death. Usually brief. Attempts to “be better” or make deals to postpone disease progression. |
| Depression | Experiencing sadness, loneliness, and a lack of motivation. Includes both reactive depression from past losses and preparatory depression from future losses and inabilities. |
| Testing | Finding different coping mechanisms. |
| Acceptance | Recognizing the inevitability of death and making peace with it. Usually the person has little or no feelings. Some persons will not reach this stage. |
Notably, there are criticisms that these stages have not been thoroughly validated and that they are “too rigid and linear.” In fact, there is no real evidence that a person goes through all these stages. These concerns were particularly valid since each person is unique and processes grief in their own way. Further, as someone approaches death, it’s easy to focus on the stages of dying, overlooking the person’s entire life experience, identify and personality.
However, this model allows us to understand that grieving is a PROCESS, hereby minimizing the stigma that accompanies grief. The knowledge of this process also increases communication and interaction during the person’s final stage of life (Amwell, 2022).
Check out this video where I discuss the best advice for someone facing death.
How do families cope with a loved one who is terminally ill?
Dealing with a loved one who is terminally ill can be one of the most difficult experiences a family can go through. In addition to the emotional toll, there can also be financial strain and logistical challenges.
However, there are ways to ease the burden and provide support for both the patient and their loved ones. One of the most important things you can do is to create a support network. This could include close friends and family, religious leaders, or professional counselors.
It’s also important to stay open and honest with communication. This can help to reduce stress and allow everyone to feel involved in the decision-making process.
Finally, it’s crucial to take care of yourself both physically and emotionally. This includes staying on top of your own health, getting regular exercise, and making time for hobbies and activities that you enjoy.
When a family is dealing with a terminally ill loved one, self-care is essential. By taking these steps, families can find some measure of peace during an incredibly difficult time.
Read also: 14 Key Tips to Help Someone Facing Death
What are the options for those who are terminally ill?
Facing a terminal illness is one of the most difficult challenges a person can face. Not only must they grapple with their own mortality, but they must also make difficult decisions about their care and treatment. While there is no single right answer, there are a few options that are commonly considered by those who are terminally ill.
One option is to continue receiving active treatment in an effort to prolong life, even if the chances of success are relatively low. Another option is to focus on comfort care, which aims to improve quality of life while accepting that death is inevitable.
Some people also choose to hasten their death through physician-assisted suicide or other means. Ultimately, the decision of how to spend one’s final days is a deeply personal one, and there is no wrong choice.

What is hospice care and how does it work?
Hospice care is a type of healthcare that focuses on providing comfort and support to terminally ill patients and their families. Hospice care can be provided in a variety of settings, including hospitals, nursing homes, and patients’ homes.
Hospice care is typically provided by a team of healthcare professionals, including doctors, nurses, social workers, and chaplains. The goal of hospice care is to help patients and their families cope with the physical, emotional, and spiritual aspects of terminal illness.
Hospice care typically includes pain management, as well as support for emotional and spiritual needs. Hospice care is usually covered by Medicare and Medicaid, as well as private insurance plans.
Final words on terminal illness
Terminal illnesses are difficult for everyone involved. The stages of a terminal illness can be confusing and overwhelming. Families cope with a loved one who is terminally ill in different ways. There are many options for those who are terminally ill, including hospice care. Hospice care provides comfort and support to both the patient and their family during this difficult time.
Do you believe that persons with a terminal illness should have a right to choose to end their life? Let me know in the comments below.
Read also: 10 Disadvantages of Spirituality You Shouldn’t Ignore
Related topics
Tips for someone facing death?
Facing death is never easy. In fact, it can be a scary experience. But, there are some things that can help make the process a little easier. It is important to talk about your feelings and fears with friends, family, or a professional.
It can also be helpful to focus on making the most of the time you have left. This may involve spending time with loved ones, pursuing hobbies, or simply enjoying the moment. Death is a natural part of life, and by accepting it and preparing for it, we can make the experience more bearable. Read more
How do I deal with grief and loss?
Grief is a natural reaction to loss. It is the process of mourning, and it is unique to each individual. There are no right or wrong ways to grieve, and there is no timetable for grief.
Some common symptoms of grief include: feeling isolated and alone, numb or disconnected from the world, angry or resentful, guilty or responsible for the death, anxious or scared, wanting to be close to others and wanting to be alone.
There are many ways to deal with grief and loss. Some people find comfort in talking with friends or family members. Others might find comfort in writing about their thoughts and feelings, or in participating in religious or spiritual activities.
Some people might choose to see a therapist or counselor to help them through the grieving process. What is important is that you allow yourself to feel whatever emotions you are experiencing, and that you find healthy ways to cope with your grief.
References
Amwell (2022)How do the five and seven stage grief models differ?
Crossroads Hospice & Palliative Care (2022) What is active dying?
Hui D, Nooruddin Z, Didwaniya N, Dev R, De La Cruz M, Kim SH, Kwon JH, Hutchins R, Liem C, Bruera E. Concepts and definitions for “actively dying,” “end of life,” “terminally ill,” “terminal care,” and “transition of care”: a systematic review. J Pain Symptom Manage. 2014 Jan;47(1):77-89.
Kintzel PE, Chase SL, Thomas W, Vancamp DM, Clements EA. Anticholinergic medications for managing noisy respirations in adult hospice patients. Am J Health Syst Pharm. 2009;66:458–464.
Perring, C (no date) Kubler-Ross and other approaches
Tyrrell P, Harberger S, Schoo C, et al. Kubler-Ross Stages of Dying and Subsequent Models of Grief. [Updated 2022 Jul 20]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-.









